Key Takeaways
- Four Medicare Savings Programs exist — Qualified Medicare Beneficiary (QMB), Specified Low-Income Medicare Beneficiary (SLMB), Qualifying Individual (QI), and Qualified Disabled and Working Individuals (QDWI) — each covering different costs at different income levels.
- An estimated 2-3 million eligible Americans are not enrolled in programs that could save them hundreds to thousands of dollars annually in Medicare premiums and cost-sharing.
- Income limits are higher than most people assume — a single person earning up to approximately $1,715/month (2025 figures, adjusted annually) may qualify for at least partial premium assistance.
- QMB is the most comprehensive program, covering Part A premiums, Part B premiums, deductibles, coinsurance, and copayments — effectively eliminating most out-of-pocket Medicare costs.
- Applying takes one visit to your state Medicaid office or a phone call to your State Health Insurance Assistance Program (SHIP) — no Medicare enrollment changes required.
Table of Contents
- The Medicare Cost Problem Nobody Talks About
- What Are Medicare Savings Programs?
- The Four Programs: Who Qualifies and What Is Covered
- Income and Asset Limits for 2025-2026
- How MSPs Interact with Medicare Advantage and Medigap
- How to Apply: A Step-by-Step Process
- Common Myths That Keep Eligible Retirees from Applying
- Extra Help with Part D: A Related Benefit Worth Knowing
- FAQ
The Medicare Cost Problem Nobody Talks About
A 65-year-old retiring today can expect to spend an estimated $165,000 in out-of-pocket healthcare costs through the remainder of their life, according to multiple industry estimates. That figure includes Medicare premiums, supplemental insurance, Part D costs, dental, and vision — but not long-term care.
For retirees on fixed incomes, Medicare premiums alone can consume a significant portion of monthly income. The standard Part B premium in 2025 is $185/month per person. Add a Part D drug plan ($30-$50/month), a Medigap supplement ($150-$300/month depending on plan and location), and Part A deductibles ($1,676 per hospital admission in 2025), and the annual cost of “free” Medicare quickly exceeds $6,000-$8,000 per person.
What many retirees — and even some financial advisors — do not realize is that the federal government operates four programs specifically designed to help lower-income Medicare beneficiaries pay these costs. They are collectively called Medicare Savings Programs (MSPs), and millions of eligible Americans never apply.
What Are Medicare Savings Programs?
Medicare Savings Programs are state-administered, federally funded programs that pay some or all of a Medicare beneficiary’s out-of-pocket costs. They are separate from Medicaid, though they are administered through state Medicaid offices. You do not need to qualify for full Medicaid to receive MSP benefits.
MSPs are designed for people who have Medicare but whose income and assets fall below certain thresholds. The programs cover different combinations of:
- Part A premiums (for those who did not qualify for premium-free Part A)
- Part B premiums ($185/month in 2025)
- Deductibles
- Coinsurance
- Copayments
Enrollment in any MSP also automatically qualifies you for Extra Help (Low-Income Subsidy) with Part D prescription drug costs — a benefit worth an additional $5,000-$6,000 per year for those who take multiple medications.
The Four Programs: Who Qualifies and What Is Covered
Qualified Medicare Beneficiary (QMB)
QMB is the most comprehensive Medicare Savings Program. It covers:
- Part A premiums
- Part B premiums
- Part A deductibles
- All Medicare coinsurance and copayments
For someone enrolled in QMB, Medicare becomes essentially free at the point of service. Providers who accept Medicare are legally prohibited from billing QMB enrollees for deductibles, coinsurance, or copayments.
Who qualifies: Individuals with monthly income at or below 100% of the Federal Poverty Level (FPL) and limited assets.Specified Low-Income Medicare Beneficiary (SLMB)
SLMB covers:
- Part B premiums only
This program helps retirees whose income is slightly above the QMB threshold but who still struggle with the $185/month Part B premium. That savings of $2,220/year can make a meaningful difference on a fixed income.
Who qualifies: Individuals with monthly income between 100% and 120% of FPL and limited assets.Qualifying Individual (QI)
QI covers:
- Part B premiums only
QI functions similarly to SLMB but covers a slightly higher income range. Funding is allocated on a first-come, first-served basis, though in practice most applicants are approved. You must reapply annually.
Who qualifies: Individuals with monthly income between 120% and 135% of FPL and limited assets. You cannot be enrolled in Medicaid and receive QI simultaneously.Qualified Disabled and Working Individuals (QDWI)
QDWI covers:
- Part A premiums only
This program serves a narrow population: people under 65 who lost premium-free Part A when they returned to work after a disability-related Medicare eligibility period.
Who qualifies: Working disabled individuals under 65 with income up to 200% of FPL.Income and Asset Limits for 2025-2026
Income and asset limits are updated annually based on the Federal Poverty Level. Here are the approximate thresholds for 2025 (2026 figures are typically released in late January):
| Program | Monthly Income Limit (Individual) | Monthly Income Limit (Couple) | Asset Limit (Individual) | Asset Limit (Couple) |
|---|---|---|---|---|
| QMB | ~$1,255 | ~$1,704 | $9,430 | $14,130 |
| SLMB | ~$1,506 | ~$2,045 | $9,430 | $14,130 |
| QI | ~$1,695 | ~$2,303 | $9,430 | $14,130 |
| QDWI | ~$2,510 | ~$3,407 | $4,000 | $6,000 |
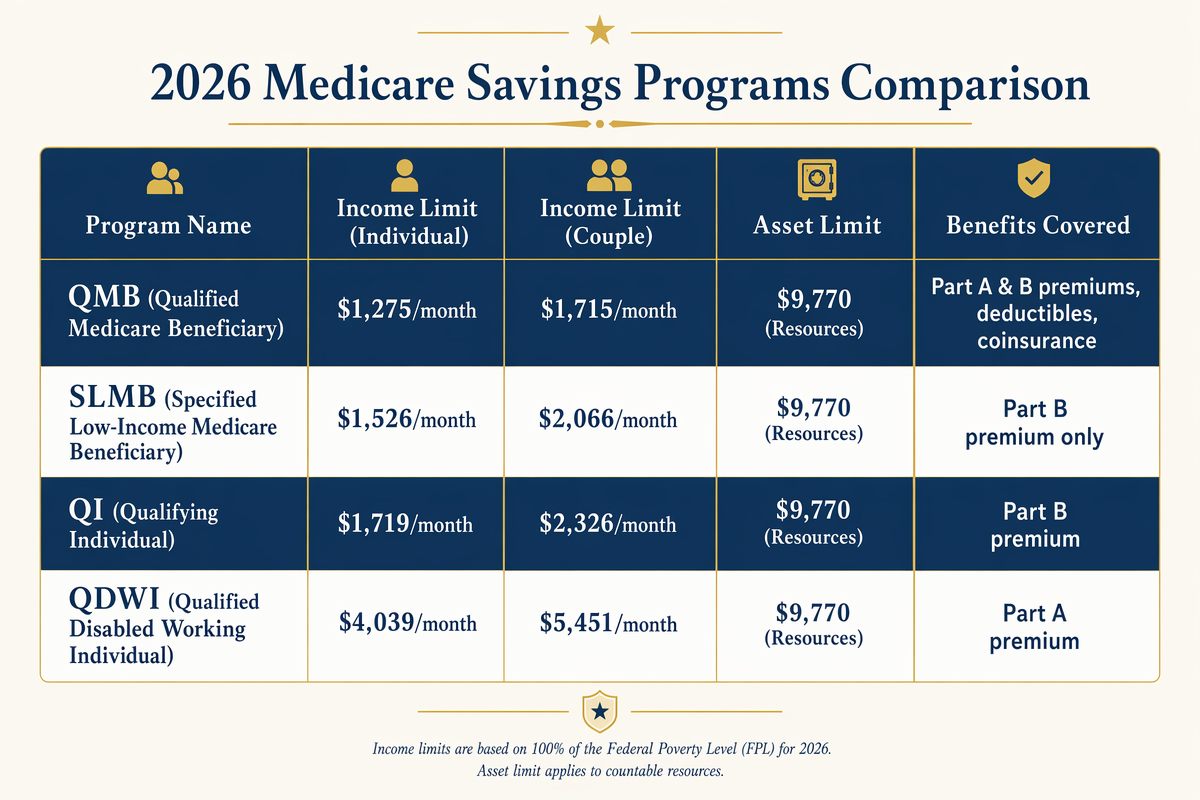
Important notes on how income and assets are counted:
- Income includes Social Security, pensions, wages, and investment income. It does not include the value of your home, one car, burial plots, or household goods.
- Asset limits count bank accounts, stocks, bonds, and cash value of life insurance (over $1,500). They do not count your primary residence, one vehicle, personal belongings, or irrevocable burial trusts.
- Some states have eliminated or expanded asset tests — check with your state Medicaid office, as eligibility varies.
In-Article Image Alt Text: Comparison table of four Medicare Savings Programs showing income limits, asset limits, and benefits covered for each program levelPro Tip: Social Security cost-of-living adjustments can push retirees just above income thresholds from one year to the next. If you were denied last year, it is worth reapplying — the income limits increase annually with inflation, and your state may have expanded eligibility.
How MSPs Interact with Medicare Advantage and Medigap
Medicare Advantage
If you are enrolled in a Medicare Advantage plan, MSPs still apply. QMB enrollees in a Medicare Advantage plan have their Part B premium paid by the MSP and are protected from cost-sharing above the plan’s limits. However, Medicare Advantage plans may have their own cost-sharing structure (copays for specialist visits, for example), and QMB protections apply to those as well — providers cannot bill QMB enrollees for Medicare cost-sharing.
Medigap
If you have a Medigap (Medicare Supplement) policy, you are paying a monthly premium for coverage that overlaps significantly with QMB benefits. If you qualify for QMB, you may no longer need a Medigap plan — QMB covers the same deductibles and coinsurance that Medigap covers. Dropping the Medigap plan could save $150-$300/month. However, be cautious: if you drop Medigap and later lose QMB eligibility, you may not be able to re-enroll in Medigap without medical underwriting (depending on your state).
Part D
All four MSPs automatically qualify you for Extra Help (also called the Low-Income Subsidy or LIS) with Part D drug costs. This reduces or eliminates Part D premiums, deductibles, and copayments. For retirees taking multiple medications, Extra Help can save $5,000 or more annually.
How to Apply: A Step-by-Step Process
Applying for a Medicare Savings Program is simpler than most people expect:
Step 1: Contact your state Medicaid office or call your State Health Insurance Assistance Program (SHIP). SHIP counselors provide free, unbiased assistance with Medicare questions and MSP applications. Find your local SHIP at shiphelp.org or by calling 1-877-839-2675. Step 2: Gather documentation. You will need:- Medicare card (or Medicare number)
- Proof of income (Social Security award letter, pension statement, tax return)
- Bank statements showing assets
- Proof of residency
Thomas’ Take: I have seen retirees assume they “make too much” without checking the actual numbers. The income limits are higher than most people expect — especially for couples. A 10-minute phone call to SHIP could save you $2,000-$5,000 per year. It is worth checking even if you think you are on the border.
Free Download: Social Security Optimization Guide
Learn the strategies that could maximize your lifetime Social Security benefits.
Get Your Free Copy
Common Myths That Keep Eligible Retirees from Applying
Myth: “Medicare Savings Programs are welfare.”MSPs are earned benefits available to Medicare enrollees who meet income and asset criteria. You paid into Medicare through decades of payroll taxes. These programs exist specifically to ensure Medicare is affordable for people on fixed incomes. There is no stigma in using a program you funded.
Myth: “I own a home, so I won’t qualify.”Your primary residence is excluded from the asset test. So is one vehicle, personal property, and burial funds. The asset test applies primarily to liquid assets — bank accounts, stocks, and bonds.
Myth: “My Social Security is too high.”Check the numbers. A single retiree receiving $1,600/month in Social Security could still qualify for SLMB or QI, saving $2,220/year in Part B premiums. Do not self-disqualify without running the math.
Myth: “The application process is too complicated.”SHIP counselors exist specifically to help with this process — for free. In many states, the application is a single form. The annual savings justify an hour of paperwork.
Myth: “It will affect my other benefits.”Enrolling in an MSP does not affect your Social Security, pension, or other retirement income. It does not require you to change doctors or Medicare plans (unless you choose to). The only change is that some or all of your Medicare costs are paid for you.
Extra Help with Part D: A Related Benefit Worth Knowing
Any MSP enrollment automatically qualifies you for Extra Help with Medicare Part D prescription drug costs. But Extra Help is also available as a standalone benefit for people who do not qualify for an MSP.
Extra Help covers:
- Part D monthly premiums (reduced or eliminated)
- Annual Part D deductible (reduced or eliminated)
- Prescription copayments (reduced to $0-$11.20 per prescription)
The income limit for standalone Extra Help is higher than MSP limits — approximately $22,590/year for individuals and $30,660/year for couples in 2025. If you take multiple brand-name medications, Extra Help can save several thousand dollars per year.
Apply through Social Security at ssa.gov/medicare/part-d-extra-help or call 1-800-772-1213.
FAQ
Can I apply for a Medicare Savings Program at any time?Yes. Unlike Medicare itself, which has specific enrollment periods, MSP applications are accepted year-round. If approved, benefits typically start the month after approval (or the month of application in some states). There is no open enrollment window to wait for.
Will MSP enrollment change my Medicare coverage?No. MSPs help pay the cost of your existing Medicare coverage — they do not change your plan, your doctors, or your benefits. If you have Original Medicare, you keep it. If you have a Medicare Advantage plan, you keep it. The only change is who pays the premiums and cost-sharing.
What if my income fluctuates year to year?MSP eligibility is reviewed periodically (annually in most states). If your income increases above the threshold, you may lose eligibility. If it drops back down, you can reapply. Some states use an annual review; others use ongoing eligibility monitoring. Report significant income changes to your state Medicaid office proactively.
Can I have a Medicare Savings Program and a Medigap policy at the same time?Yes, but it may not be cost-effective. If you qualify for QMB, the program covers the same deductibles and coinsurance that Medigap covers — so you would be paying a Medigap premium for overlapping coverage. SLMB and QI only cover Part B premiums, so Medigap would still add value if you want supplemental coverage. Review your specific situation before making changes, and be aware of Medigap guaranteed issue rights in your state.
Do Medicare Savings Programs vary by state?The four federal MSP categories and their minimum income thresholds are the same nationwide. However, some states have expanded eligibility beyond federal minimums, offer streamlined application processes, or have eliminated asset tests entirely. Your state Medicaid office or SHIP can confirm the specific rules in your state.
Help May Be Available — But Only If You Apply
Medicare Savings Programs represent one of the most underutilized benefits in the retirement landscape. The programs exist. The funding is allocated. But millions of eligible retirees never apply — either because they do not know the programs exist or because they assume they will not qualify.
For more on retirement income, bucket planning, and Social Security claiming, browse the retirement planning archive or sign up for the weekly newsletter at the bottom of any page.
This article is published by Confluence Media Group LLC, an independent publisher of educational financial content. Thomas Clark is a Series 65 Investment Advisor Representative. The information provided is for educational and informational purposes only and is not personalized financial, tax, or legal advice. Past performance does not guarantee future results. All investing involves risk, including potential loss of principal. Consult a qualified professional before making financial decisions.
Confluence Media Group LLC is a separate entity from Confluence Capital Management, the investment advisory practice through which Thomas Clark provides advisory services. Advisory services are not offered through this publishing platform.
Thomas Clark is a Series 65 licensed investment advisor and experienced trader. He specializes in investing, retirement planning, and market analysis, helping individuals build wealth and make informed financial decisions.